To demonstrate the possibility for hidden rehabilitation potential even following most severe brain injury and the uncertainty of current prognosis factors for coma and unresponsive wakefulness syndrome, we detail the rehabilitation of J. W., after coma from traumatic brain injury. Originally, with many negative prognosis factors and several medical complications, prognosis was devastating.
But, with continuing treatment, J. Improved to a high level of independence in everyday life. This shows the need for rehabilitation research to further specify the “prognostic power” of various combinations of prognosis factors, so that practitioners can come to accurate single‐case recommendations when both positive and negative predictors are present. Introduction Severe traumatic brain injury (TBI) often results in coma and subsequent disorders of consciousness such as unresponsive wakefulness syndrome (UWS) (former vegetative state), or minimally conscious state (MCS). The survival rate after a TBI, severe enough to cause deep coma and low Glasgow Coma Scale (GCS) scores, is generally poor, even in young adults. Studies show a very high overall mortality, ranging between 76% and 89%., Of the surviving patients, only very few recover to a good outcome. The majority of the survivors do so with permanent disorders of consciousness or severe disabilities (see Table ).
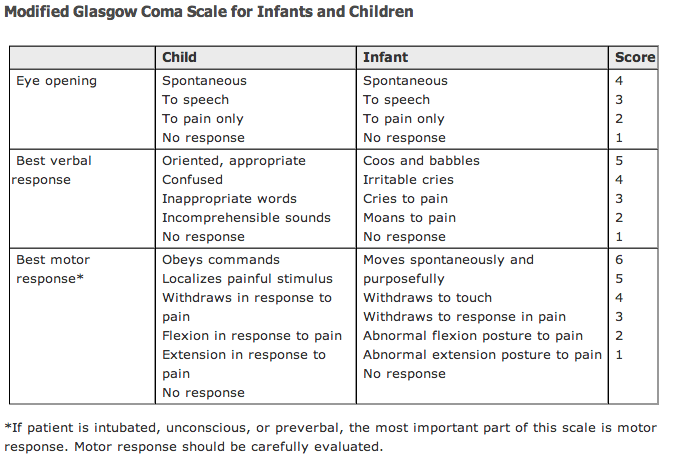
The Pediatric Glasgow Coma Scale or Pediatric Glasgow Coma Score (PGCS) is the equivalent of the Glasgow Coma Scale and is used to assess the consciousness of infants and children. Pediatric Glasgow Coma Scale is used in cases of head injury of children mostly.
In acute coma, most prognosis factors are essentially able to predict a negative outcome. Two powerful predictors, usually obtained right at the accident site, are the patient's pupillary reactions and GCS scores. Various studies report significantly increased mortality for patients with initial GCS scores of ≤5 compared to those with higher GCS scores., In fact, the chances of survival with a GCS less than 5 are considered so poor, that in regions with limited resources, patients with a GCS of ≤5 are not even admitted to intensive care units (ICU) (as reported in Jain et al.). References N/Age group Type of traumatic brain injury Initial GCS score Overall mortality Mortality with fixed pupils Mortality with low GCS plus fixed pupils Good outcome Jain et al.
102/6 to 75 years Isolated blunt head injury 3–5 76.5% 83.1% 10 patients (GOS 4 and 5) Demetriades et al. 760/from under 20 to over 55 years Blunt and penetrating trauma 3 76% 177 survivors, 18 with preinjury functional capacity Kotwica and Jokubowski 111/18–82 years Blunt and penetrating trauma 3 89% 2 patients GOS 4 2 patients GOS 5 White et al. 136/0–17 years Closed head injury ≤8 24% 93.75% of those with GCS under 5 Lieberman et al. 137/≥14 years Blunt and penetrating trauma 3 92% N = 104 100% died 11 survivors 1 patient with FIM 16 3 patients with FIM 20 Rovalis and Kotsou 345/16–70 years Closed head injuries ≤8 N = 119, GCS 3–5, 96.6% died 151 favorable outcomes, not further specified Sigorini et al. 372/≥14 years Blunt and penetrating trauma ≤15 23% 62% 279 survivors, outcome not further specified. Absent pupillary reactions are also very powerful negative predictors. Again, Jain and colleagues found that poor pupillary reactions increase the odds ratio for death to 5.5.
A combination of both, fixed pupils and a low GCS has even been found to be associated with nearly absolute mortality (96.6% and 100%). Other negative predictors (indicating death or long‐lasting UWS) obtained within the first days after the accident are the presence of hematoma on computer tomograms (CT), an age over 55 years, clinical complications (like fever or seizures), and the absence of any motor response to painful stimulation., Once a TBI‐related UWS is reached, in children, overall mortality drops (14%) but chances of an unfavorable outcome (long‐lasting UWS or severe disabilities) are still high (68%). For adults, an unfavorable outcome (death or long‐lasting UWS) of 48% is reported, only 7% reaching a good outcome., Higashi et al. Even report a mortality of 66% and only three patients (of the 110) were able to communicate at a 5‐year follow‐up. In general, a more positive prognosis is made for patients with rapid signs of recovery (within the first days and weeks) and less than 40 years of age., A more specific positive prognosis factor is an EEG reactivity to external stimulation., Such reactivity has been shown to be lacking in 92% of all patients with severe EEG slowing (. (A) Computed tomography ( CT) from the day of the accident showing acute right side hematoma with midline shift. (B) CT from 5 months after the event after cranium reimplantation showing an epidural hematoma, which required a second surgery.
(C) Event‐related potentials from an oddball paradigm at electrode Cz. Identifiable are congruent but slightly delayed N100 responses for frequent and novel tones with a peak latency of 128 msec. A discernible but delayed P300 with a peak latency at 457 msec is displayed for novels, indicating the detection and intensified processing of new and unexpected events. (D) Event‐related potentials from a N400 paradigm at electrode C4. Identifiable N100, more pronounced for semantically correct sentence endings and smaller for incorrect sentence endings. Between 400 and 800 msec, a clearly visible but delayed N400 is displayed, indicating the detection and intensified processing of semantic violations.
Rehabilitation course with all positive and negative predictors is also detailed in Table S1. During the first month in rehabilitation, the patient was still on ventilation and autonomically unstable with sweating, tachycardia, and hypertension. No change in mental status was observed. In the second month, the EEG showed severe slowing, with delta–theta dominance. Magnetic resonance imaging (MRI) displayed a right‐frontal subdural hematoma and an asymmetric, right dominant ventricle system enlargement without midline displacement, as well as parenchyma lesions with gliosis in temporal regions and in the white matter surrounding the posterior horn of the lateral ventricle. Still, by the end of the second month, J.
Could be weaned from ventilation, although there was no change in cognitive functions. By the third month, the patient reached the status of MCS. However, there were no vocalizations other than groaning to painful stimulation. No communication channel and no command following could be established.
After 4 months, a newly conducted MRI revealed considerable brain atrophy, multiple parenchyma lesions, diffuse shear lesions, but no periventricular transudation of cerebrospinal fluid. Five months after the event the cranium reimplantation was scheduled. After the operation, various complications occurred, including an epidural hematoma, which required a new surgery (see CT in Fig. No clinical improvement was apparent. After 7 months, J. Began with situation‐independent screaming.
This lasted for over 4 weeks. He screamed and moaned during his “wake” phases, which did not change with painkillers or other medication efforts. S EEG now showed an almost normal alpha rhythm.
Event‐related potentials (ERPs) for tone discrimination (P300) and semantic speech processing (N400) were clearly identifiable, albeit latency delayed (see Fig. Eight months after the event, J. Began to close his eyes on command, clinically indicating progress to MCS+. Nine months after the event, the patient established a communication channel, first via eye blink, and shortly thereafter also via nods and head shaking. Communication is described as increasingly adequate which implies that the patient improved beyond MCS. At this point, after 9 months of intensive treatment, he was sent home from early rehabilitation.
Continued on an intensive therapy program: 2 h of occupational therapy, 3 h of physiotherapy, and 2 h of speech therapy a week. He regained better body control, so that after 6 months at home, the patient was able to walk alone for about 20 m on flat ground albeit walking was still very ataxic and unstable. He also regained speech and was able to communicate adequately, although with aphasic symptoms. Epileptic seizures continued to occur about once a month. After 6 months at home, the patient was rehospitalized for 10 weeks in the rehabilitation facility (Kliniken Schmieder, Germany) to improve his gait, his memory capacity, and general independence. During this time, one and a half years after the car accident, J. Underwent a neuropsychological evaluation.
He was fully oriented, displayed normal short‐term memory, normal verbal intelligence, and average executive performance. He still showed weaknesses in reproduction of geometrical figures and text information, below‐average long‐term memory capacity, and generally slowed information processing. He continued his therapy schedule in reduced form after rehabilitation for years after the accident. Now, 10 years after the event, J. Is able to walk independently, use stairs, and even ride his bicycle again.
He has reached independence in all activities of daily living. His memory functions are still reduced but he has learned to cope. His speech is slow but his vocabulary and intonation are perfectly normal. He has communicated with the researchers personally, via telephone and e‐mail. Is employed and lives close by, but independently, from his parents. Discussion This case illustrates three points. First, good recovery is possible despite a range of powerful negative predictors (low GCS score, fixed pupils, abnormal motor findings, various medical complications, and epileptic seizures).
It should be kept in mind that every medical prognostic test is associated with “false negatives.” The prediction errors may be small for certain prognosis factors (like low GCS scores in combination with fixed pupils, ), but they are almost never 0. Even with error rates estimated to be 0%, there are usually non‐zero confidence intervals (CI) due to small sample sizes. The study of Lieberman and colleagues illustrates that fact with 104 patients with low GCS and fixed pupils: Although nobody survived, CI range was from 0.00 to 3.38. The case of J.
Highlights that very point. Second, little is known about the interaction of positive and negative predictors.
Was it only the patient's youth that outweighed all the other seemingly devastating negative predictors? Recently, attempts have been made to develop “multifactor models” for acute coma outcome. So far, these models take very different predictors into account and reach considerably different conclusions.
For example, Jain et al. Include three factors, namely the patient's pupil response, whether the patient needs ventilation right after the event, and whether the GCS improves by at least two points within the first 24 h. The IMPACT project from 2010 on the other hand, takes age, motor score, pupils, cause, CT findings, and laboratory results into account. Retrospectively inserting J. S data result in a 15% survival chance with no further specification of outcome in Jain's model, whereas IMPACT forecasts a 35% chance of favorable outcome (better than UWS). Clearly, future studies should further address the question of “prognosis profiles” of single patients and should also specify outcome levels in greater detail. This would help practitioners to come to accurate conclusions in single cases where positive and negative predictors are present at the same time.
Finally, this case illustrates the value of multimodal intensive early and late rehabilitation, as well as the usefulness of continued treatment at home and interval rehospitalization. Continuous therapy helped the patient to improve over a period of 10 years, so that now an independent life is possible.
